How can we prevent or minimise COVID-19 transmission in a clinical primary care setting?
What the research says:
The COVID-19 virus is spread primarily via respiratory droplets . Respiratory aerosols have also been implicated in viral transmission in medical settings, particularly from inhaler procedures. Droplets formed during talking, singing, coughing or sneezing remain the most common modes of transmission. The probability that brief exposure to infected but asymptomatic individuals results in viral transmission is low, although new variants may be more contagious. Prolonged (>15 minutes) and close (within 2 metres) exposure to an individual with COVID-19 infection (asymptomatic or symptomatic) is thought to more likely to result in viral transmission. Contact with surfaces contaminated with viral particles can result in transmission if the individual then touches their face. Up to 62% of transmission may occur via individuals who are asymptomatic, which includes those who are pre-symptomatic. Asymptomatic individuals and those who are post-symptomatic may remain infectious for many days.
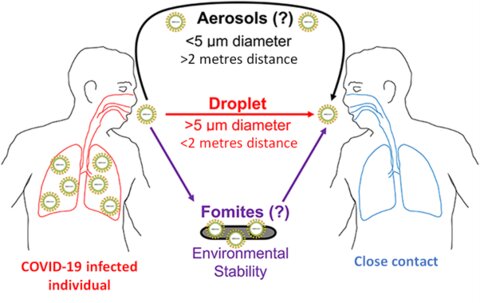
Fomite, an object or material likely to carry infection.
Source: Adapted from Galbadge T, et al. Does COVID-19 spread through droplets alone? Front Public Health 2020 https://doi.org/10.3389/fpubh.2020.00163. © 2020 Galbadage, Peterson and Gunasekera
What this means for your clinical practice:
Prevention of viral transmission is best achieved by reducing close face to face contact including maintaining at least a 2-metre distance when not conducting a physical examination, use of certified masks covering your face from the bridge of your nose to under your chin by both patients and healthcare professionals, appropriate use of personal protective equipment (PPE) including face shields or goggles, frequent hand washing and rigorous attention to ventilation and COVID-appropriate cleaning of clinical areas between patient consultations. These steps apply to all individuals presenting for healthcare. Remote healthcare consultations should be considered for all patients requiring continuing follow-up care during the COVID-19 pandemic.
Those requiring face to face consultation should be appropriately triaged to establish their risk for current COVID-19 infection. This may include remote (telephone) triaging of patients to determine likelihood of current COVID-19 infection, temperature screening prior to entry to a healthcare facility, use of PPE and social distancing. Individuals with, or at high risk for, current COVID-19 infection should be seen in a dedicated clinical area following local guidance on the use of PPE.
Resource information
- COVID-19
- Transmission
